22 Mar Endometriosis: The Silent Epidemic Every Woman Must Know About
Endometriosis affects around 247 million women worldwide, including 42 million in India — yet the condition remains underdiagnosed and poorly understood, largely because its symptoms resemble those of several other common disorders. As the best endometriosis specialist in Delhi, I see this diagnostic gap every single day — and it has to change.
So, What Exactly Is Endometriosis?
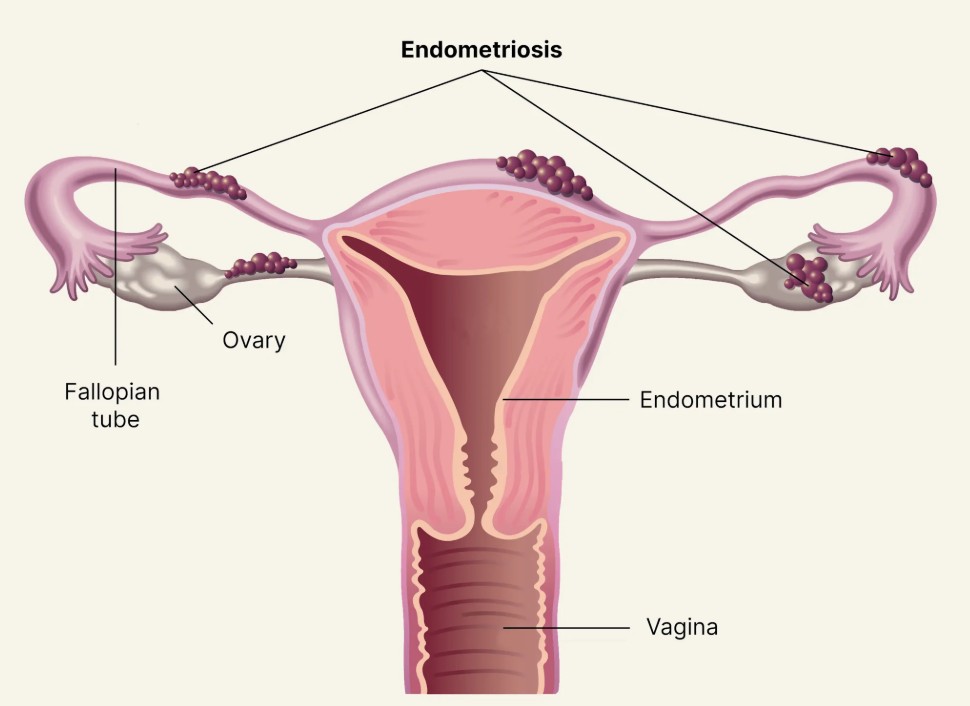
Endometriosis happens when tissue similar to the lining of the uterus — the endometrium — begins growing outside the uterus. It can appear on the ovaries, fallopian tubes, the lining of the pelvis, and in severe cases, even on the bowel, bladder, and nearby nerves.
Here is what makes it so painful: every month, just like the uterine lining, this misplaced tissue responds to hormonal changes. It thickens and breaks down — but unlike the uterine lining, it has nowhere to go. It stays trapped in the body, causing inflammation, internal bleeding, scar tissue, and adhesions that can glue organs together over time.
Endometriosis most commonly occurs in the pelvis but in some women occurs elsewhere in the body, including the abdomen and chest. It can impact sexual intercourse, bowel movements and urination, and mental health — including depression and anxiety.
The Symptoms You Should Never Ignore
Not every woman with endometriosis experiences the same symptoms. Some have debilitating pain. Others have almost none — and discover the disease only when they struggle to conceive. But these are the warning signs that should always prompt a specialist consultation:
Period pain that stops your life. Painful periods are common. Periods that leave you unable to get out of bed, vomit from pain, or require strong painkillers to function — that is not normal, and it deserves investigation.
Chronic pelvic pain. Pain that lingers throughout the month, not just during your period, is a significant red flag. Women with endometriosis suffer from dysmenorrhea, chronic pelvic pain, dyspareunia, dyschezia, fatigue, depression, and infertility — leading to significant socioeconomic impact and reduced quality of life.
Pain during intercourse. Deep pelvic pain during or after sex is one of the most commonly overlooked symptoms of endometriosis. Women often feel too embarrassed to mention it to a doctor — please don’t be.
Bowel and bladder symptoms. Pain when passing urine or stools, especially around your period, bloating, constipation, or even blood in urine or stool can all signal endometriosis involving the bowel or bladder.
Difficulty getting pregnant. Amongst women with infertility, as many as 25–50% have endometriosis. Many women first discover they have the condition when trying to conceive.
Extreme fatigue. The kind of exhaustion that sleep doesn’t fix — a total body tiredness that makes everyday life feel like a struggle.
Why Is Endometriosis Diagnosed So Late in India?
This question keeps me up at night. Women in India reported that they first experienced endometriosis-related symptoms at a mean age of 22.9 years, but the disease was diagnosed only at 29.2 years — a gap of over six years on average. All women in the study reported a lack of familiarity with the condition before diagnosis, frequent misdiagnosis with other conditions like pelvic inflammatory disease, adenomyosis, fibroids, and polycystic ovarian syndrome.
The reasons for this tragic delay are multiple. Period pain has been normalized in our culture for generations — mothers tell daughters it is something to endure, not investigate. Endometriosis affects 42 million Indian women, but less than 30 per cent know of it. Doctors sometimes dismiss symptoms as psychological or hormonal. And many women themselves feel guilty taking their pain seriously.
It needs to stop. Your pain is real. It deserves answers.
How Is Endometriosis Diagnosed?
There is no simple blood test for endometriosis — not yet. Diagnosis involves a careful, step-by-step process:
Clinical history: A detailed conversation about your symptoms, their pattern, and their impact on your life is the essential starting point.
Transvaginal ultrasound: Can detect ovarian endometriomas (chocolate cysts) and some deep disease, though it misses many lesions.
MRI pelvis: Provides a detailed map of the extent of disease, especially for deep infiltrating endometriosis involving the bowel, bladder, and pelvic nerves. Essential before complex surgery.
Diagnostic laparoscopy: Laparoscopic surgery — where endometrial tissue may be directly visualized or tissue samples removed and examined — remains the gold standard for confirming endometriosis. In skilled hands, it is also the opportunity to treat the disease in the same sitting.
Treatment: What Are Your Options?
Treatment depends on your symptoms, the stage of your disease, and whether you wish to preserve fertility.
Medical management includes hormonal therapies — oral contraceptives, progestins, GnRH analogues — that suppress the disease and provide pain relief. These work well for mild to moderate disease but do not eliminate existing lesions.
Surgical treatment is necessary for moderate to severe disease, ovarian cysts, and endometriosis-related infertility. The goal is complete excision — not just burning the surface of lesions, but removing them root and all. Incomplete surgery is one of the biggest reasons endometriosis comes back.
For complex cases involving the bowel, bladder, or deep pelvic structures, robotic-assisted surgery offers the highest precision — something I specialize in as part of my practice as the best endometriosis specialist in Delhi.
Fertility treatment: For women struggling to conceive, surgical excision of endometriosis significantly improves natural conception rates. In cases where additional support is needed, IVF or other assisted reproductive techniques can be recommended in coordination with a fertility specialist.
A Word About Your Mental Health
Endometriosis is not just a physical disease. The condition causes significant impacts including decreased quality of life, psychological effects, financial distress, strained intimate relationships, and the burden of infertility. Many of my patients carry years of being dismissed, misdiagnosed, and made to feel like they were exaggerating. That leaves a mark.
Please know — your pain is valid, your diagnosis is real, and you deserve proper care. A good specialist will treat not just your disease, but you as a whole person.
FAQs: Endometriosis — Dr. Usha M Kumar Answers
Q1. Is endometriosis the same as painful periods?
No. While painful periods are one symptom of endometriosis, they are not the same thing. Endometriosis is a complex disease involving tissue growing outside the uterus, causing inflammation, adhesions, and damage to surrounding organs. Period pain that is severe enough to affect your daily functioning, doesn’t respond to standard painkillers, or worsens over time needs specialist evaluation — it is not something to simply accept.
Q2. Can endometriosis be cured completely?
Currently, there is no permanent medical cure for endometriosis. However, with complete surgical excision of all lesions by an experienced specialist, most women achieve significant and long-lasting relief from pain. The key word is “complete” — thorough surgical removal by a skilled surgeon gives the best long-term outcomes and lowest recurrence rates.
Q3. Will I be able to get pregnant if I have endometriosis?
Many women with endometriosis — including those with severe disease — go on to have successful pregnancies. The outcome depends on the stage of endometriosis, your age, ovarian reserve, and whether appropriate surgical and fertility treatment is pursued. I take a fertility-first approach in every patient — preserving your ability to conceive is always a central part of my treatment planning.
Q4. At what age can endometriosis start?
Endometriosis can begin as soon as a girl starts her periods. About 60% of adult women with endometriosis experience symptoms before the age of 20 years, but it can take more than 12 years to reach a diagnosis from the onset of disease in adolescents. If a teenage girl is having severe, disabling period pain, she should be evaluated for endometriosis — not told to wait and see.
Q5. How do I know if my pain is “bad enough” to see a specialist?
If your period pain or pelvic pain is affecting your ability to work, study, exercise, have a normal social life, or intimate relationship — it is bad enough. You should not have to manage on painkillers every month. Come and speak to a specialist. Early diagnosis means earlier treatment, less damage, and better outcomes.
Q6. What is the difference between endometriosis and PCOS?
These are two completely different conditions that are frequently confused. PCOS (Polycystic Ovary Syndrome) is primarily a hormonal disorder affecting ovulation, causing irregular periods, excess androgen, and polycystic ovaries. Endometriosis is a disease of tissue growth outside the uterus, primarily causing pain and fertility issues. Some women can have both conditions simultaneously, which is why a thorough specialist evaluation is so important.
Q7. Why should I choose Dr. Usha M Kumar for endometriosis treatment in Delhi?
As the best endometriosis specialist in Delhi, I bring together decades of gynaecological expertise, advanced laparoscopic and robotic surgical skills, and a deeply personal approach to patient care. I understand the physical and emotional journey of endometriosis — and I am committed to giving every patient not just an accurate diagnosis and excellent surgical treatment, but genuine compassion and long-term support. My patients come to me from across Delhi, India, and abroad — trusting me with their most difficult cases.
Book a Consultation
If any of what you have read today sounds familiar — if you have been living with pain, confusion, or unanswered questions about your reproductive health — please come and see me. You deserve answers. You deserve relief.




Sorry, the comment form is closed at this time.